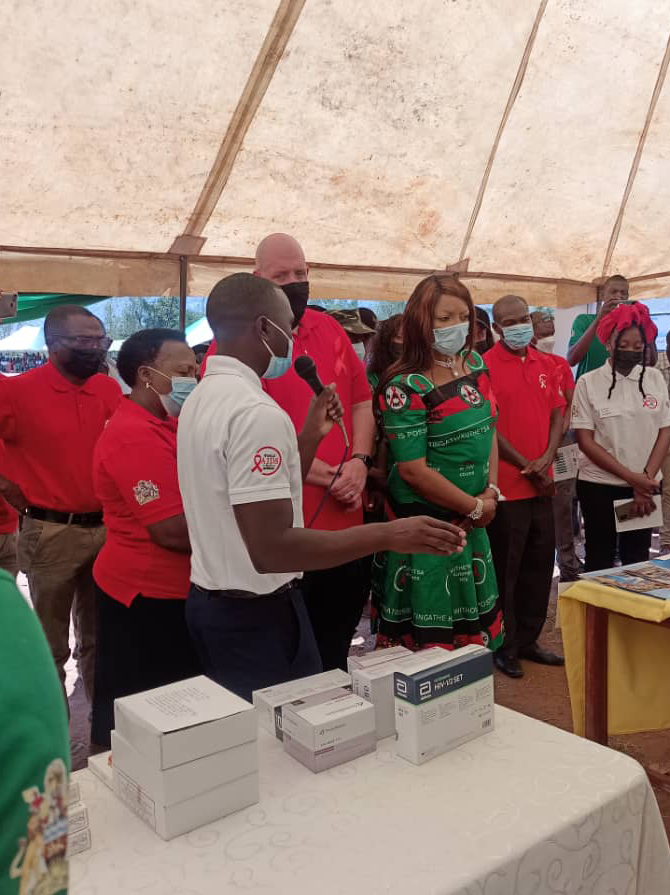
 Index testing is a is a key strategy to identify and support those most at risk of acquiring HIV.1 Within the index testing framework, exposed contacts (i.e., sexual partners, biological children and anyone with whom a needle was shared) of an HIV-positive person (i.e., index client), are elicited and offered HIV testing services.
Index testing is a is a key strategy to identify and support those most at risk of acquiring HIV.1 Within the index testing framework, exposed contacts (i.e., sexual partners, biological children and anyone with whom a needle was shared) of an HIV-positive person (i.e., index client), are elicited and offered HIV testing services.
From 2019 to 2021, the I-TECH team in Ukraine provided increased technical assistance for 39 state healthcare facilities in 11 high HIV-burden regions to advance assisted partner notification/services and index testing.
In a recently published study in BMJ Open, the I-TECH team—along with representatives from the Public Health Center at the Ukrainian Ministry of Health—describe the success of this scaled program in index testing.
“Index case testing is crucial in reaching out to exposed contacts of individuals living with HIV, notifying them, and offering HIV testing,” said Anna Shapoval, I-TECH Ukraine Country Representative. “This approach is particularly important and effective in the context of Ukrainian national HIV response where, despite numerous successes, we still struggle to close HIV testing gap and reach out to people living with HIV earlier rather than later with proper treatment and support.”
I-TECH developed exhaustive standard operating procedures for index testing; thoroughly trained healthcare teams on the index testing algorithm; as well as provided consistent and regular methodological support as part of its index testing program.
The study includes clients enrolled in index testing services in 2020, who had with both recent (<6 months) and previously established (≥6 months) HIV diagnoses. Ukraine’s physician-led model involves a cascade of steps including voluntary informed consent, partner elicitation, selection of partner notification method and follow-up with clients to ensure partners are notified, tested for HIV, and linked to HIV prevention and treatment services, as needed.
“Ukraine’s index testing services were rolled out as a standard part of Ukraine’s HIV service package at the targeted governmental health facilities, and carried out by existing physicians,” said Alyona Ihnatiuk, Strategic Information Lead for I-TECH Ukraine and lead author of the study. “At each supported facility, one or two staff members were designated as focal persons for case management and follow-up. This integrated, physician-led model was streamlined to target index cases with both recent and established HIV diagnosis, to arrive at a high number of new cases of HIV identified.”
There were 976 new cases of HIV identified through the study period, representing a yield of 19.3%, and 1,408 people living with HIV (PLHIV) have been identified throughout the two-year index testing program.
Of 14,525 index clients offered index testing, 51.9% accepted, of whom 98.3% named at least one sexual partner, injection partner, or biological child. Clients named 8,448 unique partners; HIV case finding was highest among clients with recent HIV diagnosis and among people who inject drugs (PWID), and lower among clients with established HIV diagnosis. More than 90% of all partners with new HIV diagnoses were linked to care.
“The BMJ Open study confirms that comprehensive assisted partner notification services and index testing are highly effective in identifying people living with HIV,” says Ms. Shapoval, “as well as tracing previously diagnosed partners and supporting their linkage to care. I-TECH was honored to contribute to the design and implementation of this vital intervention in Ukraine early on and see it gradually rolled out across the country with multiple partners successfully implementing it now.”
- Golden M, et al. Partner notification for sexually transmitted infections including HIV infection: an evidence-based assessment. Sexually transmitted diseases. 4th edn. McGraw-Hill; New York, NY: 2007.
THIS PROJECT IS SUPPORTED BY THE HEALTH RESOURCES AND SERVICES ADMINISTRATION (HRSA) OF THE U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES (HHS) UNDER U91HA06801, THE INTERNATIONAL AIDS EDUCATION AND TRAINING CENTER (IAETC). THE CONTENT OF THIS POST IS THE AUTHOR’S AND SHOULD NOT BE CONSTRUED AS THE OFFICIAL POSITION OR POLICY OF, NOR SHOULD ANY ENDORSEMENTS BE INFERRED BY HRSA, HHS OR THE U.S. GOVERNMENT.


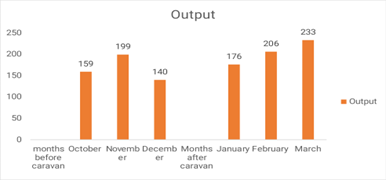

 Data from the International Training and Education Center for Health (I-TECH) program in Malawi were presented during the
Data from the International Training and Education Center for Health (I-TECH) program in Malawi were presented during the