
For many communities in the Caribbean Region, barriers to high-quality HIV treatment and care often arise before a client crosses the clinician’s threshold.
“When [key populations] access health care – and when we say key populations, we mean MSM [men who have sex with men], sex workers, transgender people – they are immediately discriminated against,” says Kenyatta Barnaby, a Key Populations (KP) Advisor working with the International Training and Education Center for Health (I-TECH) in Jamaica.
“They can’t relate to the clinician or anyone in their surroundings,” continues Barnaby, “and before they even get to [see] the clinician, there is discrimination in the waiting area.”
If a patient makes it far enough to see a clinician, the stakes become higher – misunderstandings and miscommunication can have grave consequences. Barnaby notes that, often, clients from key populations are afraid to contradict a clinician’s assumptions and may not share information that’s vital to receiving proper care.
When clients do disclose that they are gay, transgender, or doing sex work, “[a clinician] might express disgust or alarm,” explains Conrad Mitchell, I-TECH’s Key Populations Advisor in Trinidad & Tobago. “What happens directly as a result of that is that someone feels alienated, and therefore does not come back and does not get the care that they need.”
When these experiences are shared within community networks, it can result in fewer people from key population groups accessing care at facilities where others have had negative experiences.
A novel approach using real-world experiences
To address these challenges in HIV care and treatment settings, I-TECH designed and launched Improving HIV Care for Key Populations in the Caribbean, a novel preceptorship program aimed at building clinicians’ capacity to provide nonjudgmental, high-quality, comprehensive HIV care to most-at-risk communities.
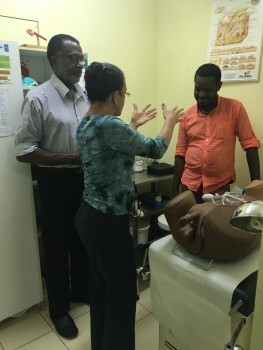
The two-day intensive training occurs in a simulated clinic setting, using targeted role-play scenarios based on real-world experiences. “Patients” are portrayed by skilled KP patient-trainers under the supervision of an experienced clinical facilitator. Clinician trainees participate in 8 to 12 different clinical scenarios featuring patients who are transgender, MSM, or doing sex work.
During these trainings, clinicians practice taking a comprehensive sexual history, performing a proper (simulated) ano-genital examination with appropriate site-specific STD screening, conducting rapid mental health screenings, and undertaking individual risk assessment and risk reduction counseling.
The program was developed and implemented by I-TECH in close collaboration with key population groups in in the region. I-TECH developed standardized case scenarios collaboratively with community members, and recruited and trained representatives from the sex worker, MSM, and transgender communities in each country to portray these scenarios as the patient-trainer and to give targeted feedback to clinicians.
Frank, face-to-face discussions
Once the trainer exits the role of “patient,” the clinician is also afforded the opportunity to have a frank and open discussion with the trainer. These conversations are wide-ranging – from the obstacles that prevent key populations from accessing care; to the health care issues they face; to psychosocial issues such as mental health, gender affirmation, gender-based violence, and substance abuse.
“One of the great things that can come out of something like this,” says Mitchell, “is although the person has come in with a physical problem, we are sensitizing the clinician to see past that.”
The patient-trainers share powerful personal stories with the clinicians, noting how small actions or expressions – such as a slight grimace or donning gloves to take blood pressure – can be interpreted as stigma. They offer insight into what runs through a patient’s mind at a health facility: fear of harassment by vendors, security staff, and other patients; anxiety around disclosing they have same-sex partners, the number of partners, or sexual practices; and reluctance to seek care for ano-genital conditions.
The patient-trainers also teach providers about the importance of using preferred names and pronouns, about avoiding the assumption of heterosexuality, and of showing a non-judgmental attitude. “A lot of it is about language,” says Barnaby. “We are equipping them with the knowledge of how to speak to a KP person without discriminating.”

A two-way street
For some clinicians, this training is the first time meeting a transgender person, or the first time receiving constructive feedback about service delivery from the perspective of the patient. Clinicians have noted that they appreciate opportunities to interact with real people from the key population groups and to get feedback on their clinical practice and interpersonal skills directly from a patient’s perspective.
Mitchell, who portrays several patients throughout the training program in Trinidad, also notes that “there is always that ‘wow’ moment with the clinicians: ‘Wow, I didn’t know this was happening.’” Mitchell says that he had a clinician admit to him that the many years of schooling that doctors go through can leave them naïve of social issues.
Perhaps most valuably, the understanding is not one-sided. At the end of the two days, says Mitchell, not only is there a marked improvement in the clinicians, but the patient-trainers come away enlightened, as well.
“Often we forget that doctors are people themselves,” he says. “I think that’s one of the things that the team in Trinidad collectively learned. Because there were a number of doctors that came to the training, and we had sort of a negative view of them…. Often what comes across as negative is this person having a rough day, a bad day, or not being able to give the kind of help they want to give.”
Barnaby echoes that sentiment, noting that a doctor can quickly get a bad reputation within the tight-knit KP communities in Jamaica, and these trainings have helped bridge the gap from both sides. “If the preceptorship trainers can see the doctor’s potential to be good,” says Barnaby, “he gets a good rep in the community, as well.”
So far the program has trained 20 clinicians from the highest volume HIV care and treatment clinics in Jamaica and Trinidad. In the coming year, I-TECH will continue to train clinicians and will also adapt the training for nurses in the region.