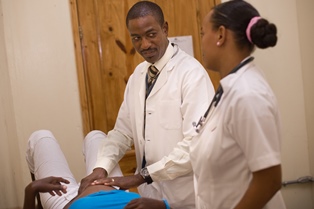
Since 2013, I-TECH has led quality improvement (QI) collaboratives in the Caribbean region, enabling multidisciplinary teams at health facilities to work toward a common goal of improving care and treatment for HIV-positive patients.
Continue reading “Continuous Quality Improvement Collaborative in the Caribbean”
Category: Caribbean
Patient-Trainers are Key to Providing High-Quality Care to MSM, Sex Worker, and Transgender Communities in the Caribbean

For many communities in the Caribbean Region, barriers to high-quality HIV treatment and care often arise before a client crosses the clinician’s threshold.
“When [key populations] access health care – and when we say key populations, we mean MSM [men who have sex with men], sex workers, transgender people – they are immediately discriminated against,” says Kenyatta Barnaby, a Key Populations (KP) Advisor working with the International Training and Education Center for Health (I-TECH) in Jamaica.
“They can’t relate to the clinician or anyone in their surroundings,” continues Barnaby, “and before they even get to [see] the clinician, there is discrimination in the waiting area.”
If a patient makes it far enough to see a clinician, the stakes become higher – misunderstandings and miscommunication can have grave consequences. Barnaby notes that, often, clients from key populations are afraid to contradict a clinician’s assumptions and may not share information that’s vital to receiving proper care.
When clients do disclose that they are gay, transgender, or doing sex work, “[a clinician] might express disgust or alarm,” explains Conrad Mitchell, I-TECH’s Key Populations Advisor in Trinidad & Tobago. “What happens directly as a result of that is that someone feels alienated, and therefore does not come back and does not get the care that they need.”
When these experiences are shared within community networks, it can result in fewer people from key population groups accessing care at facilities where others have had negative experiences.
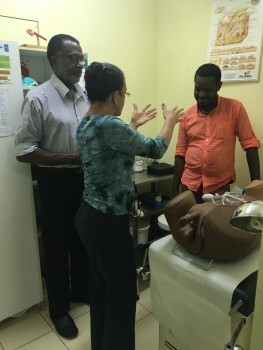
A novel approach using real-world experiences
To address these challenges in HIV care and treatment settings, I-TECH designed and launched Improving HIV Care for Key Populations in the Caribbean, a novel preceptorship program aimed at building clinicians’ capacity to provide nonjudgmental, high-quality, comprehensive HIV care to most-at-risk communities.
The two-day intensive training occurs in a simulated clinic setting, using targeted role-play scenarios based on real-world experiences. “Patients” are portrayed by skilled KP patient-trainers under the supervision of an experienced clinical facilitator. Clinician trainees participate in 8 to 12 different clinical scenarios featuring patients who are transgender, MSM, or doing sex work.
During these trainings, clinicians practice taking a comprehensive sexual history, performing a proper (simulated) ano-genital examination with appropriate site-specific STD screening, conducting rapid mental health screenings, and undertaking individual risk assessment and risk reduction counseling.
The program was developed and implemented by I-TECH in close collaboration with key population groups in in the region. I-TECH developed standardized case scenarios collaboratively with community members, and recruited and trained representatives from the sex worker, MSM, and transgender communities in each country to portray these scenarios as the patient-trainer and to give targeted feedback to clinicians.
Frank, face-to-face discussions
Once the trainer exits the role of “patient,” the clinician is also afforded the opportunity to have a frank and open discussion with the trainer. These conversations are wide-ranging – from the obstacles that prevent key populations from accessing care; to the health care issues they face; to psychosocial issues such as mental health, gender affirmation, gender-based violence, and substance abuse.
“One of the great things that can come out of something like this,” says Mitchell, “is although the person has come in with a physical problem, we are sensitizing the clinician to see past that.”
The patient-trainers share powerful personal stories with the clinicians, noting how small actions or expressions – such as a slight grimace or donning gloves to take blood pressure – can be interpreted as stigma. They offer insight into what runs through a patient’s mind at a health facility: fear of harassment by vendors, security staff, and other patients; anxiety around disclosing they have same-sex partners, the number of partners, or sexual practices; and reluctance to seek care for ano-genital conditions.
The patient-trainers also teach providers about the importance of using preferred names and pronouns, about avoiding the assumption of heterosexuality, and of showing a non-judgmental attitude. “A lot of it is about language,” says Barnaby. “We are equipping them with the knowledge of how to speak to a KP person without discriminating.”

A two-way street
For some clinicians, this training is the first time meeting a transgender person, or the first time receiving constructive feedback about service delivery from the perspective of the patient. Clinicians have noted that they appreciate opportunities to interact with real people from the key population groups and to get feedback on their clinical practice and interpersonal skills directly from a patient’s perspective.
Mitchell, who portrays several patients throughout the training program in Trinidad, also notes that “there is always that ‘wow’ moment with the clinicians: ‘Wow, I didn’t know this was happening.’” Mitchell says that he had a clinician admit to him that the many years of schooling that doctors go through can leave them naïve of social issues.
Perhaps most valuably, the understanding is not one-sided. At the end of the two days, says Mitchell, not only is there a marked improvement in the clinicians, but the patient-trainers come away enlightened, as well.
“Often we forget that doctors are people themselves,” he says. “I think that’s one of the things that the team in Trinidad collectively learned. Because there were a number of doctors that came to the training, and we had sort of a negative view of them…. Often what comes across as negative is this person having a rough day, a bad day, or not being able to give the kind of help they want to give.”
Barnaby echoes that sentiment, noting that a doctor can quickly get a bad reputation within the tight-knit KP communities in Jamaica, and these trainings have helped bridge the gap from both sides. “If the preceptorship trainers can see the doctor’s potential to be good,” says Barnaby, “he gets a good rep in the community, as well.”
So far the program has trained 20 clinicians from the highest volume HIV care and treatment clinics in Jamaica and Trinidad. In the coming year, I-TECH will continue to train clinicians and will also adapt the training for nurses in the region.
THIS PROJECT IS SUPPORTED BY THE HEALTH RESOURCES AND SERVICES ADMINISTRATION (HRSA) OF THE U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES (HHS) UNDER U91HA06801, THE INTERNATIONAL AIDS EDUCATION AND TRAINING CENTER (IAETC). THE CONTENT OF THIS POST IS THE AUTHOR’S AND SHOULD NOT BE CONSTRUED AS THE OFFICIAL POSITION OR POLICY OF, NOR SHOULD ANY ENDORSEMENTS BE INFERRED BY HRSA, HHS OR THE U.S. GOVERNMENT.
E-Learning and Data Quality Improvement Featured at CUGH 2016

The International Training and Education Center for Health (I-TECH) is presenting three posters at the 7th Annual Consortium of Universities for Global Health (CUGH) conference in San Francisco on April 9-11. The theme of this year’s conference is “Bridging to a Sustainable Future in Global Health.”
A critical component in sustainability is the ability to collect accurate and meaningful data through electronic medical records (EMRs) – the subject of two abstracts from the I-TECH Kenya team.
In addition, online learning and electronic learning (e-learning) provides opportunities for health care workers in resource-limited settings to gain critical knowledge and skills while minimizing their need to leave the workplace.
In close partnership with the University of Washington Department of Global Health’s eLearning Initiative (eDGH), I-TECH piloted e-learning modules for KenyaEMR and transitioned the HIV management diploma program at the University of the West Indies into a blended learning program that incorporates online courses.
Since 2012, the Kenyan Ministry of Health, PEPFAR, and partners have supported implementation of electronic medical record systems (EMRs) at more than 600 public-sector health facilities. The International Training and Education Center for Health (I-TECH) has supported scale-up at more than 300 of these sites.
However, implementation is just part of the story. Successful, sustained use of EMR data depends upon the knowledge and skills of front-line health care workers. To address this need, I-TECH and eDGH developed and piloted two interactive e-learning modules on EMR data quality and EMR data for decision-making.
I-TECH and eDGH found that facility staff were motivated to use EMR e-learning modules and apply what they had learned. Participants found the content relevant to their jobs and cited an interest in additional scenarios and modules. Self-paced e-learning modules were determined to be a viable solution for standardizing sustainable training on EMR systems.
To support progressive EMR data quality improvement, I-TECH developed a Routine Data Quality Assessment (RDQA) standard operating procedure and analysis tool. The RDQA procedure was defined in collaboration with the Kenyan Ministry of Health and integrated within existing policies and procedures.
From 2014 to 2015, 180 baseline and repeat assessments were conducted. I-TECH supported facility personnel to share results during county-level EMR review meetings; these presentations motivated other sites to plan for RDQAs and fostered a culture of ongoing data quality improvement. The RDQA procedure for EMR data has now been institutionalized as a method for progressively improving EMR data quality in Kenya.
In partnership with the University of the West Indies (UWI), eDGH and I-TECH transitioned a one-year diploma program in the Management of HIV Infection to a blended learning platform that combines online courses with either a clinical practicum or a research project.
The shift in pedagogy, methodologies, and technologies was achieved through a three-phased approach designed to not only train UWI faculty and staff, but also transfer online facilitation skills to them and sustain those skills.
In its second year as a blended learning online program, the diploma program has scaled up to include health care workers from Cayman Islands, Jamaica, and Suriname.
These projects are supported by the Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services (HHS) under U91HA0680, International AIDS Education and Training Center. The content and conclusions of this post are those of the authors and should not be construed as the official position or policy of, nor should any endorsements be inferred by, HRSA, HHS, or the U.S. government.
E-Learning Increases Accessibility to HIV Diploma Program in the Caribbean
Students of the graduate diploma program in the management of HIV infection have the opportunity to receive instruction from a hand-selected group of experts. Photo courtesy of Ben Depp.
In the Caribbean, an estimated 250,000 people are living with HIV (UNAIDS, 2013). To address this epidemic, health workers must have the latest information to guide the treatment and care of those living with HIV and AIDS. The University of the West Indies (UWI) St. Augustine campus in Trinidad and Tobago offers a one-year graduate diploma program in the management of HIV infection.
In partnership with UWI and the Caribbean HIVAIDS Regional Training Network (CHART), the International Training and Education Center for Health (I-TECH) and University of Washington Department of Global Health’s eLearning Program (eDGH) helped to transition the program to a blended learning platform — one that offers courses online as well as an in-person practicum.
Support for this transition was provided by the U.S. President’s Emergency Plan for AIDS Relief (PEPFAR) through the Department of Health and Human Services’ Health Resources and Services Administration (HRSA).
The program recently completed its first semester in this new format. With the expanded platform, students have the flexibility to access the course material “anytime and anywhere,” says Professor Zulaika Ali, Program Coordinator, “and it allows students to organize their training around their routine activities, which is important for mature working individuals.”
The conversion of courses online creates a one-of-a-kind program in the Caribbean, increasing access for mid-career health professionals working in the public sector, for non-governmental organizations (NGOs), and for commercial organizations. The program was designed for medical doctors, pharmacists and dentists, as well as nurses with bachelor degrees from any recognized university; registered nurses with a minimum of three years of experience; social workers; management staff from government ministries, private sector and NGOs; and tutors and lecturers in training institutions.
After a week-long online student orientation, students explore the following topics through online instruction and relevant resources, synchronous virtual classroom sessions, and collaborative activities and discussions. At the end of each semester, students complete an in-person exam. After completion of the online courses, students participate in an in-person practicum or dissertation. Courses include:
- Research Methods and Design
- HIV Epidemiology and Pathogenesis
- Laboratory Techniques for Diagnosis of HIV
- General Management of HIV/AIDS
- HIV Co-Infection and Other Related Issues
- HIV Health Systems
- Sexual and Reproductive Health
In addition to the flexibility this part-time program offers, students also have the opportunity to receive instruction from a hand-selected group of experts from around the globe, including professors, health care workers from the Ministry of Health and NGOs, and professionals practicing in the region.
Transition from in-person to blended learning
In late 2013, I-TECH and eDGH were approached by UWI to convert the in-person diploma program into its second, blended rendition. The team started by piloting two courses online in the Moodle learning management system (LMS). From there, they obtained critical feedback for the remainder of the conversion.
Their research showed that students felt the course content was clear, appropriate, interesting, and applicable to their work and reported a preference for recorded lectures and relevant videos, anytime/anywhere access, and interactions with instructors and peers. Likewise, faculty enjoyed building new skills through online instruction.
“We conducted two in person, on-site faculty workshops, countless Skype calls, online trainings, and emails to build the capacity of faculty to develop and teach online,” says Elizabeth Scott, Senior E-Learning Developer with eDGH. “Working with faculty was a highly rewarding experience. They were motivated and dedicated, and they worked tirelessly side-by-side with us to create the best possible experience for students.”
As part of the project, the I-TECH/eDGH team also developed a commercial for the program (see below), as well as a number of introductory materials that can be used for a variety of online and blended learning programs. Among them are a general student orientation to help learners identify skills and characteristics necessary for success in online courses and an e-learning basics module for instructors.
“The informational materials developed for the program will help to improve the delivery of health care more generally,” says Dr. Ali.
A robust transition guidebook was also assembled, containing roles and expectations, best practices, online orientation materials, processes, budgeting templates, evaluation tools, job aids, and tasks and timelines for faculty and staff for ease of handover from year to year.
“The delivery of this program in the blended format will have a tremendous impact on the quality of care delivered to people infected with and affected by HIV,” says Dr. Ali. “The Faculty of Medical Sciences looks forward to welcoming regional and international students into the program. This new platform will surely enrich the learning experience of all involved.”
Collaborative Creates ‘Culture of Quality Improvement’ in Jamaica
A JaQIC team’s storyboard illustrates inspiration points and accomplishments on the journey toward quality improvement. Storyboards are a creative way for teams to learn from one another.
Despite strong clinical capacity, systemic barriers may prevent local care teams from executing CD4 count and HIV viral load tests. These tests are critical for monitoring the health of people living with HIV — and their response to antiretroviral therapy (ART).
In response to this challenge, in October 2013, ten treatment sites from the four Regional Health Authorities kicked off the Jamaica Quality Improvement Collaborative, or JaQIC (Ja-quick).
The collaborative is led by the International Training and Education Center for Health (I-TECH), in partnership with the Caribbean HIV/AIDS Regional Training Network (CHART), and supported by the U.S. President’s Emergency Plan for AIDS Relief (PEPFAR) through the U.S. Health Resources and Services Administration (HRSA).
The project is coordinated by I-TECH Senior Quality Improvement Advisor Shay Bluemer-Miroite, with Dr. Chris Behrens, Clinical Associate Professor of Medicine, Family Medicine & Global Health at the University of Washington, serving as clinical advisor.
“The aim of the project was to significantly increase CD4 and viral load testing by March 2014, and it succeeded in that in all ten sites,” said Bluemer-Miroite, noting that within six months, JaQIC was seeing measurable results. (In fact, from baseline to March 2014, sites improved incidence of CD4 testing by up to 34 percentage points.)
“But,” she added, “the collaborative has achieved so much more than that.”
Working Together to Improve Quality
Building on the existing investment in training and capacity development, quality improvement collaboratives such as JaQIC empower frontline health care workers to implement best practices and improve quality of care.
They also rely on the knowledge of existing clinical care teams, who are most familiar with health systems challenges and best positioned to identify solutions to resolve them. These challenges run the gamut from the availability of patient forms, to problems with transport of samples, to equipment failures during sample processing.
Through the collaborative, sites identify potential problems that can crop up at each step in the process, test these ideas via plan-do-study-act (PDSA) cycles, and share learning. As JaQIC teams gathered during a series of Learning Sessions to “share seamlessly, steal shamelessly,” they not only improved the quality of care, they also built excitement for quality improvement and demonstrated that frontline staff can make impactful changes.
Far-Reaching Impact
“Programs struggle with obtaining the data to prove that they are having an impact,” said Bluemer-Miroite. “Through the collaborative, tracking data became particularly meaningful to the health care teams – because they were the ones who were using the data. By tracking patient-level data from the outset, it’s easy to see how the quality of care is being affected, and it increases the data quality, too.”
The success of the program has led to the buy-in of the Jamaican Ministry of Health (MOH) – so much so that the MOH has added the role of QI Coach to its Treatment, Care and Support Officers (TCSOs), and all of the collaborative’s activities will fully transition to the MOH in December.
The collaborative has also spread to four additional countries in the Caribbean (CaReQIC): Trinidad and Tobago, Barbados, the Bahamas, and Suriname, which have joined a new group from Jamaica to form CaReQIC. While gearing up for CaReQIC Learning Sessions, coordinators realized that more foot soldiers would be needed to liaise with the sites directly, so I-TECH helped to develop training for a cadre of QI Coaches in all five countries.
The effects of this program will be far-reaching, even after its transition.
“What’s really exciting about JaQIC is its potential for a sustained impact on multiple levels,” said Dr. Behrens. “JaQIC has dramatically increased rates of CD4 and viral load testing via systemic changes that are likely to persist into the future. More importantly, however, JaQIC has introduced a ‘culture’ of quality improvement in the region that has been enthusiastically adopted across a broad spectrum of local and regional stakeholders.”